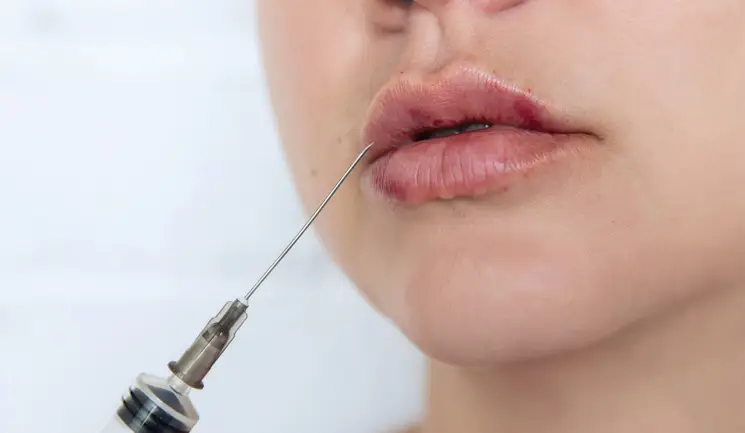
Dr Martyn King provides an introduction to differentiating between a bruise and a vascular occlusion when performing dermal filler treatments
To access this post, you must purchase Aesthetics Journal Membership – Annual Elite Membership, Aesthetics Journal Membership – Annual Enhanced Membership or Aesthetics Journal Membership – Basic Membership.
log in
log in