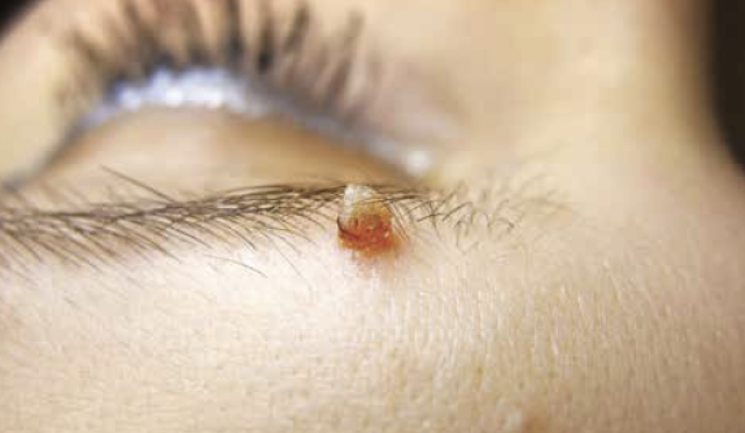
Dr Paul Charlson discusses the use of cryotherapy for benign dermatologic concerns in aesthetic practice and how it can benefit both your patients and business
To access this post, you must purchase Aesthetics Journal Membership – Annual Elite Membership, Aesthetics Journal Membership – Annual Enhanced Membership or Aesthetics Journal Membership – Basic Membership.