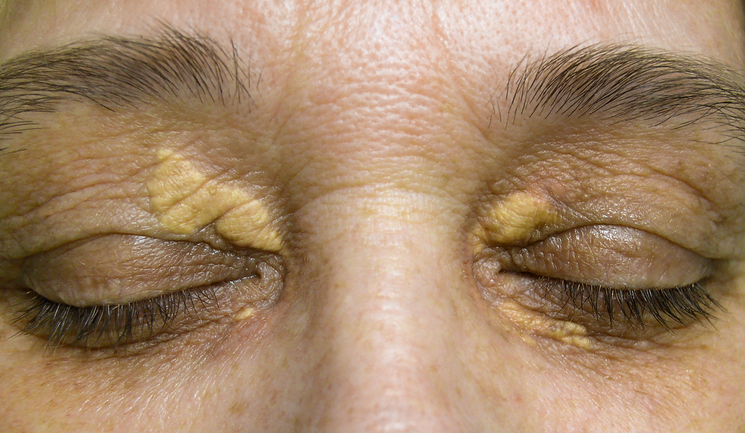
Dr Firas Al-Niaimi explores the aetiology and treatment options for the dermatological condition presenting on patients’ eyelids
To access this post, you must purchase Aesthetics Journal Membership – Annual Elite Membership, Aesthetics Journal Membership – Annual Enhanced Membership or Aesthetics Journal Membership – Basic Membership.