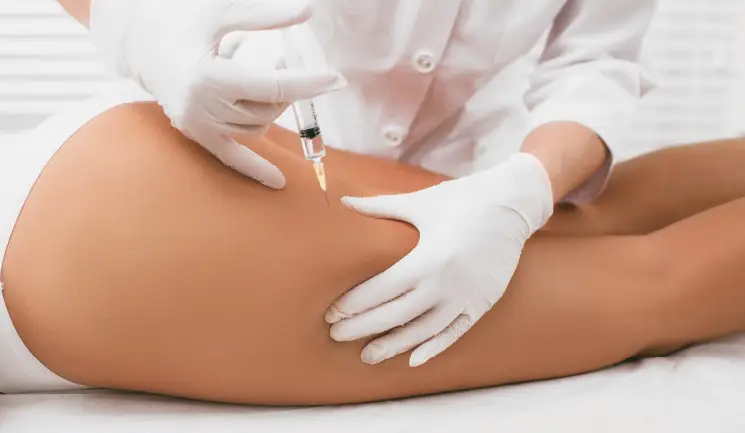
Dr Olha Vorodyukhina and Dr Tracy Xu explore the possible adverse effects following deoxycholic acid injections for fat reduction and present a patient case study
To access this post, you must purchase Aesthetics Journal Membership – Annual Elite Membership, Aesthetics Journal Membership – Annual Enhanced Membership or Aesthetics Journal Membership – Basic Membership.
log in
log in