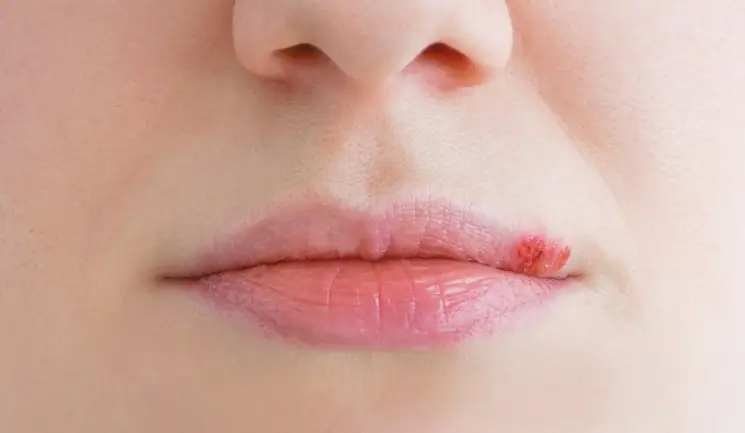
Dr Natalie Geary discusses how to diagnose herpes simplex virus in your patients and what to consider before injecting
To access this post, you must purchase Aesthetics Journal Membership – Annual Elite Membership, Aesthetics Journal Membership – Annual Enhanced Membership or Aesthetics Journal Membership – Basic Membership.
log in
log in