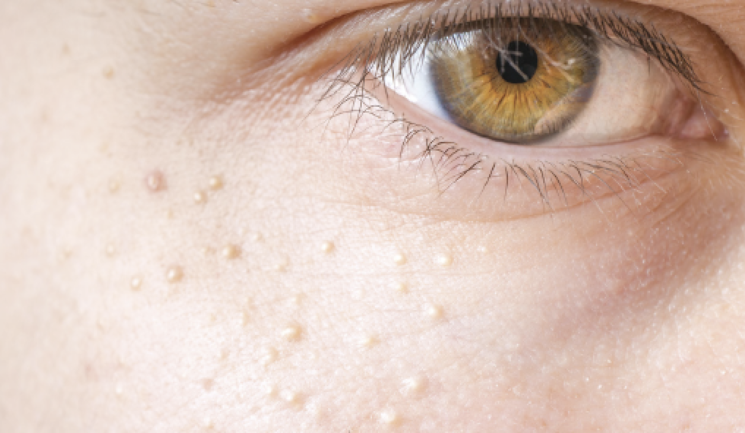
Independent nurse prescriber Louise Walsh provides insight into the different types of milia and shares methods of treatment and prevention
To access this post, you must purchase Aesthetics Journal Membership – Annual Elite Membership, Aesthetics Journal Membership – Annual Enhanced Membership or Aesthetics Journal Membership – Basic Membership.